Prostate Cancer Treatment Options in the Willamette Valley
There’s no longer a one-size-fits all treatment plan for prostate cancer. It's good to know your options and choose what's best for you.
Prostate cancer is usually a slow-growing cancer, so it may not require treatment right away. Take the time to understand how advanced your cancer is and talk with your oncologist about your options. When it comes to prostate cancer, there are many factors to consider. These include the Gleason score determined during the biopsy, the stage of prostate cancer which indicates how far it has spread, the grade of the cancer which tells the doctor how quickly it will grow, the patient's age and their overall health condition. Your oncologist will guide you through what steps would be best for you.
Common Prostate Cancer Treatments
Treatment options may include one or a combination of the following:
Active Surveillance of Prostate Cancer
If detected before the cancer has spread outside of the prostate, immediate treatment may not be necessary. Active surveillance may be the best choice to start. This is typically a period of time that can range from several months to several years where your PSA will be monitored every few months by the oncologist who is watching for a steady incline in PSA levels. Another biopsy may be done periodically as well to see if the cells have progressed further away from healthy cells.
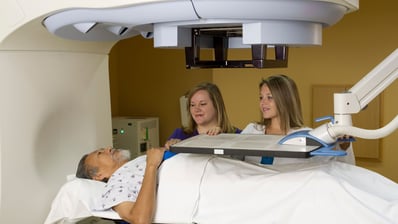
Precise Radiation Therapy for Prostate Cancer Treatment
Advances in technology have given radiation oncologists and technicians the ability to pinpoint prostate cancer and avoid or minimize damage to surrounding healthy tissue during radiation treatment.
Radiation therapy is an option for men with prostate cancer at any stage. Men with early-stage prostate cancer may choose radiation therapy instead of surgery. It can also be used after surgery to destroy any cancer cells that remain in the area. Men with prostate cancer in later stages can benefit from radiation treatment to relieve pain.
Before treatment, your radiation oncologist will use CT simulation to map the precise location of the prostate and the tumor, which makes it possible for the doctor to specify which area to treat and areas to avoid.
Hypofractionated Radiation Therapy for Prostate Cancer
Traditionally patients needed to come to the cancer center five days a week for at 6-8 weeks to complete their radiation therapy treatments. A recent approach called hypofractionated radiation therapy, or hypofractionation, allows the oncologist to deliver the total dose of radiation therapy in a shorter time period. With hypofractionated radiation therapy, the same results can be achieved in 4-5 weeks. This is done by giving a higher dose of radiation at each treatment.
The specific number of treatments depends on where the cancer is located, its size, and the patient’s overall health. This shorter treatment time is possible using advanced technology that precisely aims rays of radiation at the cancer cells. This delivery method allows the cancerous cells to be treated with a higher dose while sparing nearby organs and tissues.
Related Reading:
Treating Prostate Cancer In Less Time With Advancements in Therapy
.jpg?width=398&name=treating-prostate-cancer-in-less-time-advanced-treatments-wvci-cancer-doctors%20(1).jpg)
Intensity Modulated Radiation Therapy (IMRT) with SmartArc
Our bodies, including cancer tumors, are three-dimensional. Using a system called SmartArc, doctors can deliver IMRT directly to the prostate in a single rotation around the patient, for precise and efficient treatments.
“It is highly computer-controlled radiation, and we can very carefully control where the radiation goes and where it doesn’t go,” says Dr. Fryefield.
SmartArc treatments typically take between 50 - 60% less time to deliver than standard IMRT.
At WVCI, we use SmartArc and Calypso technologies to deliver radiation very precisely to the cancer cells while avoiding healthy tissue.
Image-Guided Radiation Therapy (IGRT)
Tumors move in the body, and organs shift. IGRT utilizes frequent imaging during a course of radiation therapy, tracking changes in the patient’s body that may shift the exact location of the cancer.
“We take a CAT scan of the patient each day prior to treatment,” says Dr. Fryefield. “We find out where the target is, set the treatment up in a very precise manner, and then deliver the radiation in a controlled way. The combination of all those things leaves the patient with fewer side effects.”
IGRT is used in conjunction with Intensity Modulated Radiation Therapy (IMRT), such as in Calypso where electromagnetic transponders are implanted into the prostate for ultra-precise radiation treatment delivery.
Stereotactic Body Radiation Therapy (SBRT)
At WVCI, we were the first in the valley to treat using SBRT for prostate cancer. SBRT kills prostate cancer cells while minimizing exposure to surrounding, healthy tissue by using advanced imaging techniques to deliver a high dose of radiation that is directed to a tumor with millimeter precision.
Traditionally, patients with localized prostate cancer would undergo surgery or eight to nine weeks of radiation therapy. For prostate cancer patients who meet specific criteria and have appropriate indications, SBRT is administered in five sessions, as opposed to 45.
“Stereotactic body radiation therapy (SBRT) really designates that someone is going to get about five treatments,” explains Dr. Thomas Sroka, a radiation oncologist at WVCI. “That’s given over about two weeks, versus classic radiation therapy for prostate cancer, which is given over nine weeks.”
SBRT is a promising option for patients who have early-stage prostate cancer. This technology may also be used to treat medically inoperable tumors or tumors that have recurred after previous radiation treatments.
"There's fewer treatment sessions, possibly less side effects, and equal outcomes as those who would come for 8-9 weeks of therapy, " adds Dr. Sroka.
When patients undergo radiation therapy, it’s common for them to ask: What will it feel like?
At Willamette Valley Cancer Institute, we deliver a variety of radiation treatments using the Trilogy Linear Accelerator by Varian Medical Systems. Its powerful, advanced motion management capabilities make it possible to treat tumors with precision and efficiency.
“Typically, patients are amazed after their first few treatments, because it’s kind of like getting an X-ray,” says WVCI radiation oncologist Dr. David C. Fryefield. “You lie on the table, you don’t move and the machine rotates around you.”
The radiation is stronger than that used for an X-ray, but the procedure is painless. Each highly targeted treatment lasts only a few minutes, although the setup time—getting you into place for treatment—takes longer.
Patients often ask if radiation treatment will make them sick or make their hair fall out. The answer, Dr. Fryefield says, is no.
“The radiation only goes where it’s supposed to go. The goal is to hurt the cancer and keep the healthy tissue happy.”
At WVCI, an expertly trained team, lead by the patient’s radiation oncologist, creates a customized, individualized plan of treatment for each patient.
With today’s advanced techniques, the side effects of radiation treatment are usually minimal and will recede.
Patients don’t feel anything during treatment, and because there are no immediate side effects patients are able to drive to and from their treatment sessions.
Side effects happen over the course of a few weeks, and the extent depends on the individual and the area being treated.
Our team of prostate cancer experts plays a vital role in planning your treatment.
Our medical dosimetrist is highly skilled and trained to understand how radiation oncology treatment machines and equipment work and have the expertise needed to generate radiation dose distributions and dose calculations in collaboration with our medical physicists and your radiation oncologist.
We have three physicists who oversee the technical aspects of your radiation therapy and who supervise quality assurance and radiation safety procedures by checking each radiation plan and running it through a series of safety checks before our radiation therapists administer the radiation treatments.
Related Reading:
What Are My Prostate Cancer Treatment Options Other Than Surgery?
What happens if prostate cancer returns after radiation or surgery?
If your prostate-specific antigen (PSA) numbers rise after a definitive therapy, such as surgery or radiation, for most patients, there will be no other evidence of the disease. That’s good news because, in most cases, treatment is unnecessary right away.
If your PSA is rising, a bone and CAT scan is usually ordered to see whether the cancer has spread. If the prostate cancer does spread, the vast majority of cases show in the bones first, then the lymph nodes or abdomen. But this scenario is fairly uncommon when doctors see PSA rising after therapy.
With a slow-rising PSA, your oncologist will track it over time and perform periodic scans to find any cancer growth. It’s not a “sit back and watch” approach. Rather, with active surveillance, the doctor looks at very precise measurements over time to monitor changes.
For most patients, checks happen every two to three months. But all treatment plans are individualized to the patient’s case and comfort level.
Systemic Therapies for Prostate Cancer
Hormone Therapy
When your doctor is ready to treat a high PSA, the first intervention is typically Lupron, a drug that lowers testosterone levels, which cancer feeds on.
There are two possible ways to take Lupron: intermittently or continuously. The data shows that continuous Lupron is slightly better than intermittent Lupron, but the side effects are more significant. The best course of action is to individualize.
Individualized treatment plans are the most important aspect of cancer care, as our understanding of cancer has advanced and the treatments have become more focused on specific abnormalities.
Hormonal medicines are more specific in the enzymes they target, which means fewer side effects and a more effective treatment. There are also new medicines and molecular drugs that target specific proteins that cancer cells rely on to grow.
Chemotherapy
Chemotherapy is rarely the first option, even when a large mass is found. There are now a multitude of options before chemotherapy is recommended.
Before you make a decision, we recommend that you seek several opinions and review your options. We are here to help you learn the facts, know your options and choose what’s best for you.
The Latest Treatments for Prostate Cancer Available at Willamette Valley Cancer Institute
If you have been diagnosed with prostate cancer, the next step is to schedule a consultation with a prostate cancer doctor. At Willamette Valley Cancer Institute (WVCI), we offer personalized treatment plans using the latest technologies available, as well as second opinions.
Prostate Cancer Specialists Caring for Patients in the Willamette Valley and the Oregon Coast
WVCI prostate cancer centers provide patients with the latest in prostate cancer treatments. Select a location that is convenient for you to request a consultation with an oncologist.
