If you recently had a polyp removed or you had surgery to remove a tumor from the colon, the pathologist who reviewed the tissue under a microscope will provide analysis in a report. The most significant information in the report is whether the tissue samples were cancerous.
If the samples show that cancer is present, becoming familiar with the terms on the report will help prepare you for your first meeting with a cancer specialist called an oncologist.
What is a Colon Pathology Report?
A colon pathology report is a medical report created by a pathologist – a doctor who specializes in studying tissue and fluid samples to diagnose illnesses. In addition to determining the presence of cancer, it can also identify other aspects of the tumor, such as the grade, the type of polyp, and whether the cancer is invasive.
Pathologists put their findings into a report given to your doctor for review. You may also receive a copy for your records.
Colon Pathology Reports Terminology
The terminology used in colon pathology reports is usually more familiar among medical community members than it is to patients. You might see several words repeated throughout your pathology report that you wouldn’t know otherwise. Below are some common medical terms listed on your colon pathology report.
Parts of the Colon
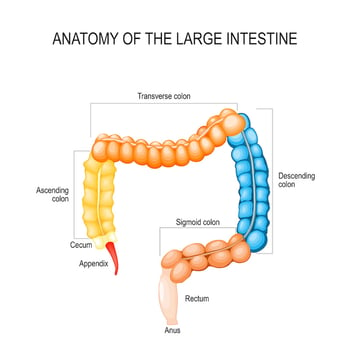 The colon (large intestine) may be subdivided into several parts and described in this manner on a pathology report: cecum, ascending colon, transverse colon, descending colon, and sigmoid colon.
The colon (large intestine) may be subdivided into several parts and described in this manner on a pathology report: cecum, ascending colon, transverse colon, descending colon, and sigmoid colon.
The cecum is the beginning of the colon, where the small intestine attaches to the large intestine. The ascending, transverse, and descending colon are all parts of the colon after the cecum. The sigmoid colon is the end portion of the colon that connects to the rectum, the area that holds waste until you have a bowel movement.
Mucin
Mucin is a lubricant produced by the colon. Some types of colon cancers create a large amount of mucin. These types of cancer are called mucinous or colloid adenocarcinomas.
Polyps
Polyps are growths found in the lining of the colon. If the pathologist tests a polyp, a description of the type will be provided.
Invasive
Invasive or infiltrating are terms to describe cancer spread beyond the lining of the colon.
Differentiation and Colon Cancer Grade
Differentiation refers to the cancer grade and explains how abnormal the cells look. The grade, which the oncologist will assign based on the information gathered from the pathology report, will impact the type of colorectal cancer treatment needed.
Colon cancer grades fall into three categories:
- Well-differentiated (low-grade)
- Moderately differentiated (intermediate-grade)
- Poorly differentiated (high-grade)
Typically, higher-grade and poorly differentiated cancer spreads faster than other grades.
Dysplasia
Dysplasia describes changes in cells detected in the colon. Cell changes can range from low-grade to high-grade depending on how abnormal they look under a microscope.
- Polyps that have low-grade (mild or moderate) dysplasia are only mildly abnormal, meaning they don’t look much like cancer.
- Polyps that have high-grade (severe) dysplasia are more abnormal and look more like cancer.
A follow-up colonoscopy may be needed sooner for patients with high-grade dysplasia than it would for those with low-grade dysplasia.
Understanding Types of Colon Polyps
Your pathology report may discuss types of polyps found in the colon.
Adenomatous polyps, the most common type, are made of tissue that looks like the normal inner lining of your colon or rectum. However, when looking at them under a microscope, the pattern in which they grow becomes visible:
- Tubular - most common.
- Villous - more common in a larger polyp. This type tends to have features resembling a finger or a leaf.
- Tubulovillous - many adenomas have a mixture of both growth patterns, so they are called tubulovillous adenomas.
Other types of polyps include sessile and serrated. Sessile polyps are flattened and broad. Serrated polyps have a saw tooth pattern when viewed under the microscope. Serrated are more likely to be precancerous rather than cancerous.
Genetics of Colorectal Cancer
If the biopsy indicates cancer, the pathologist may perform biomarker testing to see if a specific genetic mutation is fueling the cancer. These are not hereditary genetic mutations but rather mutations that occur over the course of the patient’s lifetime.
Your report may refer to tests that closely examine changes, known as gene mutations, in the KRAS, NRAS, and BRAF genes. Typically, these types of tests are for people who have colon cancer at a later stage. The results of these tests help your doctor determine which type of treatment plan is right for you.
Check out our blog: Colorectal Cancer: Why Are More Younger People Being Diagnosed?
MSI, MSH2, MSH6, MLH1, PMS2 Testing
Sometimes, other tests reflected on your pathology report may show an abnormality known as microsatellite instability (MSI) in the cancer cells. When this happens, the oncologist will likely recommend additional genetic testing to see if you have tested positive for Lynch Syndrome. Having Lynch Syndrome puts you at higher risk for colon cancer and other types of cancer. Knowing the results of these tests will determine what treatment you receive and how aggressive it should be.
Next Steps After a Pathology Report Shows Colon Cancer
It’s not uncommon to have questions about your pathology report. The best way to get the answers you need is to speak with an oncologist who specializes in colon cancer. At Willamette Valley Cancer Institute, our team of colorectal cancer specialists is ready to help you understand your diagnosis and create a personalized treatment plan based on the findings in the report and other tests to determine the extent of cancer.
We also offer second opinions, which can be helpful if you have a pathology report for a colon or rectal cancer diagnosis but don’t understand what it means. Most insurance plans cover appointments for second opinions.
If you live in and around Willamette Valley, request an appointment with one of our colorectal cancer doctors for a consultation. We have cancer centers in Albany, Corvallis, Eugene, Lincoln City, Florence, and Newport, Oregon, to help meet your needs close to home.